Dr. Rathin Datta
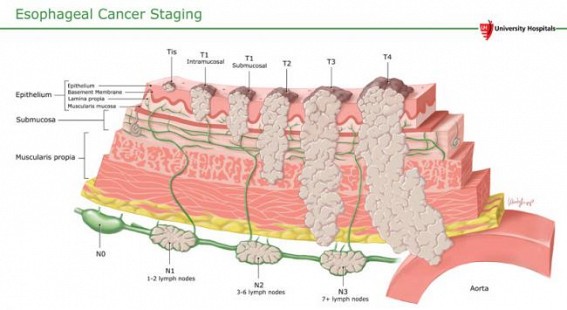
PHOTO : Esophagus Cancer staging process.
Esophagus [USA] or the Oesophagus [ UK] is the muscular tube in the human body that connects the throat with the stomach. Cancer of the Oesophagus had been my nemesis; not that I did not study the subject well or did less than the rest, far from it, in fact I had spent more time than the rest in mustering the lesion, I have begged help from others too often.
My batchmate in the Royal College of Surgeons used to laugh at me. Eva i.e. Dr. Prof.EvaDastoor, the Parsi thoracic Surgeon from Bombay was herself a highly skilled thoracic Surgeon with vast experiences in Oesophageal Surgery, used to opine that my knowledge about this lesion was as good as her and always asked me to shake off my inferiority complex as I had gathered adequate experience by participating in no less than 40 such surgical procedures.ie esophagectomy, performed by master-surgeons.
By the time it was nineties, I had been retired from Govt. service in Tripura as the Chief Advisor in Surgery to the Govt, and had switched over to two large private hospitals in Calcutta. It was still called Calcutta in ‘92,the two large hospitals where I parked are Peerless Hospital and Ruby General Hospital ,the OTs were modern and were decently equipped and was staffed with skilled personnel, where I could wipe out the sad memories of the couple of DOTs(death on table) that I was carrying.
Prof.Eva my batch mate in the RCS Edinburgh, had also retired from her hospital in Bombay(now Mumbai) and was spending couple of years in Calcutta. My wife Dr Swapna Datta was a specialist in Maternity and Child Welfare & was the Deputy Director in the Health Dept of Tripura. After taking VRS from the Govt. service she had joined a reputed NGO in Calcutta(CINI) as the Consultant.
One of her Paramedic i.e. Health Visitor Sulagna was having increasing difficulty in swallowing and consulted me.
Barium Swallow had revealed Rat tail filling defect of the esophagus and endoscopy/biopsy was positive for Squamous cell carcinoma of the lower third of esophagus. The PET test confirmed that there was no distant metastasis in her body of the tumor and was therefore an ideal case where chances of a full cure were bright.
Her relations, wanted to double check, wanting a second opinion, they were told a second opinion was welcome but for heaven’s sake no delay please! Patient returned after a week, wanting us to do the surgery.
Esophagectomy is a very complex surgical procedure requires, 4 to 8 hour of hard and very delicate dissection, preferably by highly skilled General Surgeons, well trained for the job or thoracic surgeons, or preferably by a team of both.
Now-a-days, the minimally invasive Surgery is in vogue. We had already co-participated in a few thoracic procedures and had started looking for a suitable case of operable Ca esophagus till Sulagna appeared on the scene with a provisional diagnosis of Carcinoma, of the lower third of Esophagus confirmed, after Barium swallow X-ray showing a “irregular Rat tail deformity”, endoscopy and biopsy was done by me and histopathology of tissue taken during endoscopy[esosophagoscopy] confirmed the diagnosis of “Squamus cell carcinoma”. The positive thing was the negative PET finding which ruled out any distant spread i.e. in liver.
“How about doing an esophagus?” Prof Eva would ask to tease me & my reply would be “why not mate? Find one”. She knew about my weakness and was fond of teasing me.
Sulagla’s case was in a platter. She has confirmed Squamous cell carcinoma of the lower third of the Esophagus and luckily for the patient PET test was negative confirming absence of any spread outside the esophagus, an ideal case for surgery and of good chance of a cure.
Non-invasive surgery (MIS) is employed now a days, but that was in 1993, the classical approach was planned i.e. Transthoracic Approch. A very skilled anesthetist was also essential for the team and was available. He with one of his juniors joined our team.
Mrs Sulagna Das, the patient in her early fifties, was bold and knowledgeable and exactly knew what was wrong with her and was ready to face the ordeal. Our two OT nurses were good and confirmed they were used to my speed.
Dr Bose was a good anaesthetist, employed a one lung anaesthesia spared the left lung which remained collapsed all along the procedure, gave us undisturbed space to function.
The transthoracic approach and Prof.Eva’s skill. Given the Diathermy knife Eva zoomed in through the 8th rib bed ,on way excised the 8th rib and went through the rib bed, extended the incision right across to the right rectus abdominis muscle, entered the chest cavity and abdomen simultaneously obtained a wide exposure of thoraco-abdomen, a even wider exposure was obtained after retracting the left lung and the left lobe of the liver to the right.
The tumor in the form of an spindle was identified, apparently .there was no spread, no secondary nodes beyond the organ. Prof. Eva’s knowledge of the anatomy was amazing, clear conception of the tissue layers were also amazing.
Though I was a faster operator, she was more accurate, sure of the layers, quickly dissected the esophagus from its bed identifying the spindle shaped growth from the surrounding tissues along with a strip of the pleura and pericardium covering the furiously beating heart and the Aorta.
She freed the esophagus right up to the upper third, freeing it from the heart and the aorta, divided it across, an extremely difficult work done with great skills. Her hands and fingers moved like a Belle dancers—a joy to watch!
I, the general surgeon took over from there; for the abdominal part of the esophagectomy:-
Mobilizing the stomach and the abdominal esophagus was not difficult. The left gastric artery was divided along with some of its branches to elongate the stomach. Also divided was the terminal part of the Gastroepiploic artery branches and the short gastric arteries and some of the splenic branches moving the spleen away.
Thus freed, stomach was elongated made into a narrow tube, divided the stomach right across the upper end, made the upper end of the stomach looking like a tube and was pulled up in the thorax, removed the growth en-bloc and joined up the two cut ends to establish continuity. The large wound was closed in layers with a drain.
The post operative recovery was smooth but training the patient to learn swallowing the food took time. We handed over to the Radiotherapist and the Chemotherapist after two weeks, when the patient had been stabilized
Sulagna recovered well, went back to her work as the paramedic in the NGO. She would regularly attend the follow up clinic.
It was the second week of December 2002,in the community hall of the Golf Towers complex where we live in Kolkata, it was the ‘Sradh’ ceremony of my wife Swapna. Swapna had lost her fight against GIST (Gastrointestinal Stromal Tumor) a sure killer malignant lesion, A familiar voice wished me. It was Sulagna, 8 years after her surgery was looking great, had come to pay last respect to her senior colleague in the NGO
(Names changed for privacy)
Dr. Rathin Datta, FRCS (England, Edinburgh & Glasgow).FFIMS (Athens)
Surgeon & Sports Medicine Specialist, Retd. Chief Advisor of Surgery, GB & VM Hospitals, Govt of Tripura
Padmashree Awardee, winner of the Bangladesh Liberation war honour
This article also published in Facebook www.facebook.com/tripurainfoway simultaneously.
To send your appreciation and comments pl. send email to editor@tripurainfoway.com or tripurainfoway@gmail.com or Post Online below.
- Why Modi’s BJP swept key India regional elections
- TIWN’s landmark legal victory against BJP Govt’s Illegal attacks to shutdown fearless Media
- India to be world's third-largest economy by 2030 -S&P Global Ratings
- Tripura's Dark Era : Mafia style Brutal attacks on Journalists, fight for your Citizen rights !
- How to access tripurainfoway.com via HOLA from India



